Assessment of hypercoagulability in dogs with ischaemic brain infarcts
10 July 2024
Sophie Wyatt and Stefano Cortellini received a PetSavers grant in 2022 to investigate platelet aggregation and coagulation status in dogs with ischaemic brain infarct.
An ischaemic brain infarct, otherwise known as an ischaemic stroke, arises following the sudden interruption of blood flow in a vessel supplying part of the brain. Ischaemic stroke is a major cause of morbidity and mortality in the human population, and due to increased awareness and availability of advanced imaging modalities, it is diagnosed with increasing frequency in canine patients too.
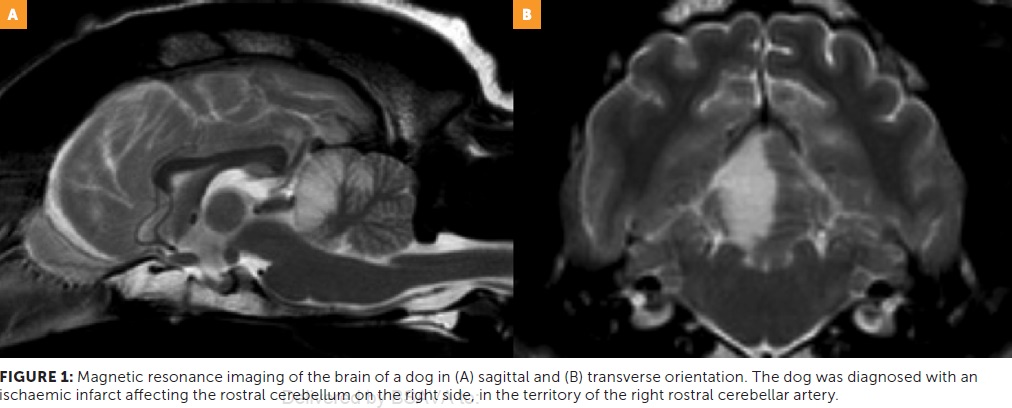
Whilst canine stroke patients have historically been thought to have a good prognosis, death or a poor long-term outcome has been reported in up to half of affected dogs. Additionally, up to one third of dogs may experience recurrence of neurological signs. Therefore, given the guarded prognosis in some cases, further research is urgently needed to improve our management. Specific therapies are currently lacking, and treatment is aimed at supportive therapy and management of underlying conditions when identified.
What are the current knowledge gaps?
The pathophysiology of canine ischaemic stroke is poorly understood and likely multifactorial but blood stasis, endothelial dysfunction, and hypercoagulability have been proposed. The association with ischaemic stroke and hypercoagulability has recently been explored but, to date, platelet function has not specifically been evaluated in canine stroke patients, and literature regarding assessment of the coagulation status is sparse. Previously, over half of canine ischaemic stroke patients were identified with a concurrent condition such as chronic kidney disease and hyperadrenocorticism; interestingly, these cases also had a worse outcome evidenced by death, failure to improve, or disease recurrence. A relative hypercoagulable state and thrombosis may therefore be a manifestation of underlying disease which is an important factor when considering the pathophysiology of the condition.
A recent consensus statementregarding anti-thrombotics in veterinary critical care recommended the use of anti-thrombotic therapy in ischaemic stroke in the presence of a disease known to be a risk for thrombosis; however, evidence in support of this is weak. Thromboembolic disease and endothelial dysfunction linked to cardiovascular disease and secondary platelet activation is a common mechanism in human stroke patients. As such, anti-thrombotic therapy forms part of the standard of care in most human stroke patients to reduce the risk of recurrence and improve long-term outcome. This raises the question whether anti-thrombotic therapy has a role in canine cerebral vascular incidents (CVIs) too.
Research
The aim of our study is to investigate platelet aggregation and coagulation status in dogs with ischaemic stroke, utilizing the techniques of viscoelastic measurement and platelet impedance aggregometry. Furthermore, we will investigate the association between hypercoagulable state and short- and long-term outcome including disease recurrence, as well as any association with concurrent disease in dogs with ischaemic stroke. The study will run over a 3-year period during which all canine patients diagnosed with ischaemic stroke at the study institution will be invited to enrol. Follow-up information will be obtained via re-examination and an owner questionnaire. Therefore, as part of the study, all enrolled dogs will be offered two free-of-charge re-examinations.
How might the research benefit other dogs?
By exploring the association between coagulation status and outcome/underlying conditions in canine ischaemic stroke patients, we hope to address a key knowledge gap regarding disease pathophysiology. Rather than relying on anecdotal evidence, the results of this study will be used to inform decisions regarding anti-thrombotic therapy and anticoagulation, with the hope of improving case outcome. The study will also provide detailed case outcome information which may provide prognostic data, allowing veterinarians to better guide owners when contemplating difficult management decisions for their pets. Finally, study findings may have translational benefits to the field of human medicine in which ischaemic stroke is a growing health burden.
Case recruitment
Enrolment of affected cases is the main challenge to the study at present. This is largely associated with limited availability of methods for evaluating platelet aggregation and the time frame in which this must be measured relative to case presentation, which limits the study to a single centre. We would welcome referral of any cases with suspected ischaemic stroke (i.e., presenting with (per)acute clinical signs localized to the brain and non-progressive beyond 48 hours) to the Queen Mother Hospital for Animals, RVC, via: s.wyatt@rvc.ac.uk.
Acknowledgements
We are extremely grateful to PetSavers for the invaluable funding opportunity, as well as Petplan Charitable Trust who have partly funded the research. The research detailed in this article was approved by the Clinical Research Ethical Review Board based at the RVC (URN 2021 2090–2). We would like to thank the team at the Queen Mother Hospital for Animals (QMHA) for their help with case recruitment and follow up. Huge thanks also to the RVC blood donors, their owners, and the QMHA transfusion team.
About the author
 Sophie Wyatt
Sophie Wyatt
Sophie graduated from the Royal Veterinary College (RVC) in 2012. Following this, she worked in small animal general practice, as well as carrying out overseas veterinary charity work in volunteer posts based in Fiji and Greece. Sophie returned to the RVC to complete a 1-year rotating internship, followed by a neurology-specific internship at Pride Veterinary Referrals. She then completed an ECVN neurology residency programme at the RVC in 2020, after which she became a European Specialist and an RCVS Specialist in Veterinary Neurology. Sophie currently works as a lecturer in neurology and neurosurgery based at the RVC.
